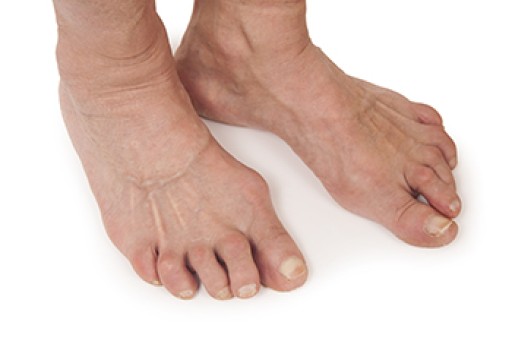
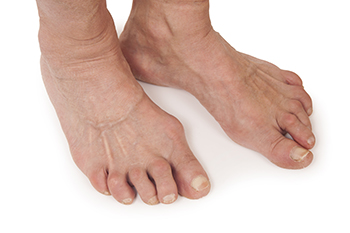
Arachnodactyly, commonly known as spider fingers, is a condition that is characterized by unusually long and slender digits in the hands or feet. When this condition affects the feet, it results in notably elongated and thin toes. It is often an inherited condition and can be a standalone feature or part of a broader genetic disorder, such as Marfan syndrome or Ehlers-Danlos syndrome. These syndromes involve connective tissue disorders that can lead to a range of physical abnormalities, including arachnodactyly. In the context of foot health, arachnodactyly can sometimes cause discomfort or difficulty in finding properly fitting footwear. While the condition primarily affects the appearance of the feet, it typically does not impair foot function or mobility. However, it can be associated with other foot-related issues, if part of a broader syndrome. Management of arachnodactyly primarily involves addressing any associated conditions and wearing comfortable and supportive footwear. If you have this condition, it is strongly suggested that you have regular appointments with a podiatrist for monitoring.
Some foot conditions may require additional professional care. If you have any concerns, contact one of our podiatrists of Associates in Podiatry, PC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Rare Foot Conditions
The majority of foot conditions are common and can be treated by a podiatrist. Standard diagnostic procedures are generally used to identify specific conditions and treatment can be rendered. A podiatrist also treats rare foot conditions which can be difficult to diagnose and may need extra attention and care.
There are many rare foot conditions that can affect children. Some of these can include:
- Freiberg’s disease
- Kohler’s disease
- Maffucci syndrome
Freiberg’s disease - This can be seen as a deterioration and flattening of a metatarsal bone that exists in the ball of the foot. It typically affects pre-teen and teenage girls, but can affect anyone at any age. Symptoms that can accompany this can be swelling, stiffness, and the patient may limp.
Kohler’s disease - This often targets the bone in the arch of the foot and affects younger boys. It can lead to an interruption of the blood supply which ultimately can lead to bone deterioration. The patient may limp or experience tenderness, swelling, and redness.
Maffucci syndrome - This affects the long bones in a child’s foot leading to the development of abnormal bone lesions. They are benign growths and typically develop in early childhood and the bones may be susceptible to breaking.
A podiatrist can properly diagnose and treat all types of rare foot conditions. If your child is affected by any of these symptoms or conditions, please don’t hesitate to call our office so the correct treatment method can begin.
If you have any questions please feel free to contact our offices located in Pittsburgh-South Hills, and Pittsburgh-Bellevue, PA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.